Reflections from Rural Practice at StreeArogya Rural Foundation by
Dr. Priya A. Chauhan, MD
Gynecologist & Founder Director
For 35 years, my clinical practice as a gynaecologist in Denmark was inseparable from the ultrasound machine. In Scandinavia, the vaginal ultrasound probe is often described as an extension of our fingers during a per vaginal examination. It allows immediate evaluation of the uterus, ovaries, fallopian tubes, and urinary bladder — ensuring prompt diagnosis and timely treatment. In most Scandinavian countries, ultrasound training is extended beyond specialists. Nurses and certified sonographers perform standardised obstetric scans, allowing gynaecologists and obstetricians to focus on clinical decision-making and treatment.
At the recent 2025 conference of FIGO World Congress of Gynaecology and Obstetrics, I attended sessions on AI-assisted ultrasound diagnostics. These innovations enhance detection of complications such as intrauterine growth restriction and congenital anomalies — without replacing clinical judgment. Globally, technology is expanding access.
Yet in rural India, access is narrowing.
The PCPNDT Act: Ethical Intent, Practical Barriers
The Pre-Conception and Pre-Natal Diagnostic Techniques (Prohibition of Sex Selection) Act, 1994 — commonly known as the PCPNDT Act — was enacted to combat sex-selective practices and address India’s historically skewed sex ratio. Its purpose is vital and morally justified.
However, the implementation of the Act has created unintended barriers in rural healthcare delivery.
Key legal provisions include:
Section 3 – Prohibits the use of prenatal diagnostic techniques except for specified medical purposes and mandates registration of all ultrasound facilities.
Section 4 – Permits prenatal diagnostic procedures only under defined medical indications and requires detailed documentation for every case.
Section 5 – Mandates written consent of the pregnant woman and strictly prohibits communication of the sex of the fetus.
Section 29 – Requires maintenance and preservation of complete records, with severe penalties for deficiencies, including suspension or cancellation of registration.
While designed to prevent misuse, these provisions regulate all ultrasound machines — including those used for non-obstetric gynaecological indications.
In practice, the administrative burden, fear of punitive action, and procedural rigidity have limited the full utilization of ultrasound in rural centres, even when scans have nothing to do with pregnancy or sex determination.
The Ground Reality at SARF
At Stree Arogya Rural Foundation (SARF), our mission is to provide preventive and evidence-based healthcare to rural women.
When I returned from Denmark to serve in rural Maharashtra, I could not imagine practicing without ultrasound. Together with my husband, a radiologist, we invested in a machine for our rural center.
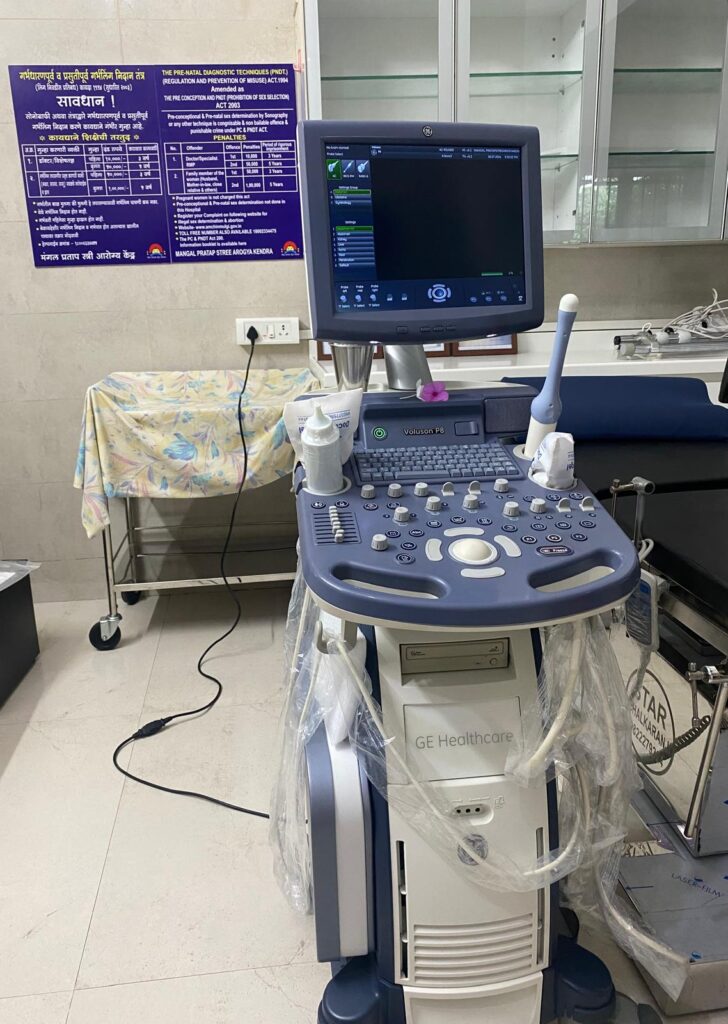
The process of obtaining PCPNDT registration was lengthy and complex. Since we are physically present only periodically, the machine must be sealed and locked in our absence.

Recruiting a radiologist or gynaecologist to work full-time in a rural area is extremely challenging. Furthermore, registering additional doctors under PCPNDT involves extensive procedural requirements. The law restricts scanning authority largely to specific specialists.
Meanwhile, our colleague, Dr. Kusum Moray (MD Community Medicine and Family Medicine), has observed and assisted in numerous supervised scans. With structured training, she could competently perform a gynaecological ultrasound for non-obstetric purposes. Yet regulatory barriers prevent this.

The result is a diagnostic tool that remains underutilized — while women wait.
The Women Who Are Affected
The women who come to SARF travel long distances. Many cannot afford repeat visits.
When ultrasound access has been available, we have:
• Detected early-stage breast malignancy
• Diagnosed uterine abnormalities like fibroids etc.
• Monitored ovulation during infertility treatment
• Evaluated abnormal uterine bleeding and pelvic pain
These scans are unrelated to fetal sex determination.
Yet the current framework does not sufficiently distinguish between ethical gynaecological care and misuse linked to sex selection.
The consequence is delayed diagnosis.
Delayed treatment.
And preventable suffering.
A Balanced Way Forward
This is not a call to weaken the PCPNDT Act. The protection of the girl child must remain non-negotiable.
However, thoughtful reform is necessary:
• Differentiation between obstetric and non-obstetric ultrasound
• Structured certification pathways for trained rural physicians
• Simplified documentation processes without compromising accountability
• Use of digital tracking systems to enhance transparency
Several states, including Karnataka, have begun reconsidering restrictions on trained MBBS doctors performing ultrasound under defined conditions. Such reforms deserve careful evaluation at the national level.
Ethical protection and healthcare access must not be mutually exclusive.
A Call to Action
At SARF, we believe that rural women deserve the same diagnostic dignity as women anywhere in the world.
We call upon:
• Policymakers to reassess implementation barriers under Sections 3, 4, and 29 of the PCPNDT Act
• Public health experts to support differentiated regulatory models
• Medical councils to create structured rural ultrasound training programs
• Civil society and donors to support advocacy and capacity-building initiatives
If you believe in strengthening rural women’s healthcare through ethical, evidence-based reform, we invite you to join our journey.
Support our work.
Engage in dialogue.
Advocate for balanced policy change.
Partner with us in expanding safe and responsible access to essential diagnostics.
Because protecting the girl child and empowering the woman must go hand in hand.
Legal Disclaimer
This article reflects professional and field-based observations and does not constitute formal legal advice or official interpretation of the PCPNDT Act. Readers are advised to consult statutory authorities or qualified legal professionals for legal clarification.


3 thoughts on “When Regulation Restricts Care: Rethinking Ultrasound Access Under the PCPNDT Act”
Commendable work envisioned and carried out, Priya. The very best to your team to overcome red tape and to continue your good work
Thank you Ma’am, for your encouraging words.
Thanks Uma 🙏🏾